A routine ENT appointment turned tonsillectomy
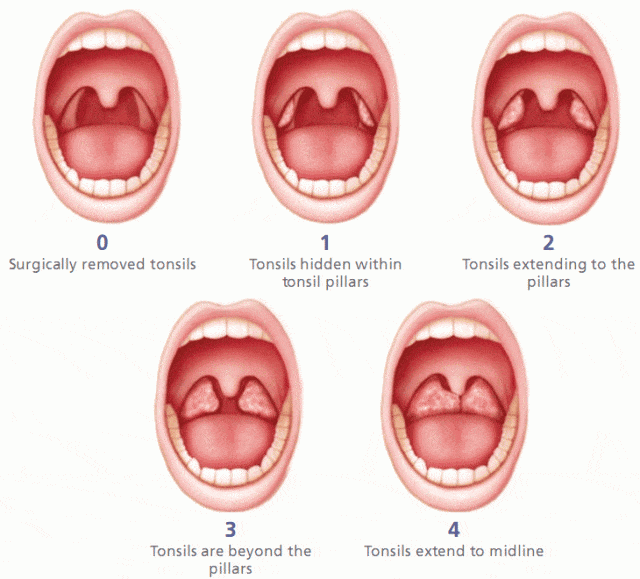
I took Charlie to an ENT specialist this morning. He apparently has sleep apnea and it’s gotten worse lately. Basically, he snores at night and he even “snores” when he’s awake! I didn’t expect an instant solution from this appointment, maybe just some suggestions for how to help clear his nasal passages in some way. To my surprise, the specialist knew within a minute what was causing Charlie’s issues. Indeed, his tonsils are so big that they touch each other. Check out the chart below! Charlie has level 4 tonsils so he needs a tonsillectomy.
What happens at night when his muscles relax is that his throat closes and causes him to gasp for air. It’s affecting his quality of sleep and therefore impacting his quality of life too. There’s no doubt Charlie’s tonsils have to come out. His surgery is in 4 weeks.
Tonsillectomy and mixed emotions
I’m so conflicted about this. I’m happy there’s a solution to Charlie’s breathing issues, but, well, Charlie will have to go under general anesthesia AGAIN! It’s always a nerve-wracking experience. Modern medicine is safe but zero risk doesn’t exist. Surgery always sucks whether your child is neurotypical or not but with Charlie, there are even more risks.
The worst part for me as his mom is that Charlie doesn’t understand any of this. That moment when he wakes up from general anesthesia, he’s always angry and confused. When he looks at us it feels like he’s thinking, “why did you let them do this to me?”
The fact that his receptive skills aren’t strong enough for him to understand what’s going on sucks. We can’t explain that we’re doing it to help him, and it makes this whole thing even harder on everybody. Then there are care instructions for post-surgery healing that will be impossible to communicate to Charlie. I’m afraid Charlie will think we don’t love him for putting him through this.


Autism, regression, and anxiety
Additionally, Charlie will be missing at least a week of therapy. Questions are rushing through my head… What if he has a regression from the general anesthesia and lack of therapy? There’s no study linking general anesthesia and autism but Charlie’s autism symptoms peaked a month after he was put under for the first time. While my rational side knows it’s just a coincidence, general anesthesia scares me. Not to mention, Charlie’s throat will be raw and in pain for two weeks. What if he forgets how to talk or chooses not to talk again because he’ll associate talking with the pain?
Last but not least, the doctor said Charlie’s voice will change. I don’t want his sweet little voice to be any different, the little voice that said mama for the first time a few weeks ago…
Ultimately, I know we’re doing the right thing. It’s all going to be okay, and anyway, it has to be done. I’m just hoping the surgery will go smoothly and the recovery without stress. Ice cream for two weeks, right?? My mom will be here the week following Charlie’s surgery. She’s coming from France with Tom, my step-dad. I haven’t seen them in two years. Exciting! And plus, having them here to help out with Charlie while he’s feeling down will be great, and we’re happy to have them.


![[Autism] This Holiday Season, We Celebrate Our Differences 5 autism mom blog reindeer in here tradition](https://theautismcafe.com/wp-content/uploads/2019/11/9-1-520x400.jpg)


4 Comments
Gloria
2018-04-13 at 12:21 AMHello Eileen
I am a pediatric nurse in the PACU( (post anesthesia care unit) of a Children’s Hospital. We recover many children after T&A surgery. Some of the children are in the autism spectrum. A child life specialist prepares the children and parents in the pre op area with pictures, doll play and toys. This is done with parent permission. In the PACU the patients usually come out with an IV in place, used for hydration, pain and anti nausea medications. With the autistic children, we try to take the IVs out ASAP, have parents at the bedside ASAP, and have something familiar for the children from home when they wake up, like a special stuffed animal, a blanket, a specific toy the child has with him/her all the time, etc.
So I guess my point is, if you go to a pediatric hospital with pediatric anesthesiologist and pediatric nurses, we are very aware And empathetic to the needs of asperger/autistic children. We are also very aware of parental concerns and anxieties. Our bedside nursing practice is to take care of not only the patient but the family as well.
Sarah
2022-03-29 at 7:10 PMI am a $N and I too have a 3 year old with ASD ..and wanted to just send my appreciation and gratitude. I just wanted to say it’s makes me proud to be a nurse – when I see such heartwarming (yet such professionalism) replies to post such as yours, it’s that heroism that nurses are known for, not for the, seemingly “big acts” but those different (not smaller acts) of many, many acts of kindness, empathy, understanding, without judgmet and the pure ‘want’ to help in all different ways – Like your comment is an example of those different but so sincere ways that a lot of nurses like yourself do without even thinking about it – that natural impulse to just care and be able to help in any way you can. Nurses are truly Born and not made acts of selflessness and a tru want to make the world a better place – makes being a nurse all that more amazing.
Sarah Ramsell
2022-03-29 at 7:12 PMOPPps apologies – spelling error I’m an RN (Reg Nurse)
Sheila
2022-03-18 at 8:45 PMHello! Thank you for sharing this wonderful story. Could you please elaborate on the therapy Charlie did? My lb is three and has recently been diagnosed. I would like him to access some therapy.